For patients living with advanced heart failure, being told they are not eligible for a heart transplant can feel like the end of the road. But new research suggests that, for many, this may not be the final answer.
A study published in the Journal of Cardiac Failure – Intersections shows that with the help of a left ventricular assist device (LVAD) and coordinated medical support, many patients can overcome barriers and eventually qualify for a life-saving transplant.
In This Content
A Second Chance at Transplant
Heart failure remains a major global health challenge. In 2022 alone, it contributed to over 425,000 deaths in the United States—accounting for nearly 45% of all cardiovascular-related fatalities.
Despite heart transplantation being the most effective treatment for advanced cases, not every patient qualifies immediately. Eligibility often depends on various medical, lifestyle, and social factors that can impact surgical outcomes and long-term recovery.
The encouraging news? Some of these barriers are not permanent—and that’s where LVAD support comes in.
Understanding the Barriers
Before being approved for a transplant, patients undergo a detailed evaluation. Several factors can make someone temporarily ineligible, including:
- Age: Higher risks are associated with patients over 70
- High BMI: A body mass index above 35 increases complications
- Substance use: Active smoking or drug use can harm a new organ
- Chronic conditions: Diseases like diabetes must be well controlled
- Psychosocial challenges: Lack of stable housing or caregiver support
While some limitations—like age—cannot be changed, others such as weight, lifestyle habits, and disease management can improve over time. These are known as modifiable barriers.
The Role of LVAD: A “Bridge to Decision”
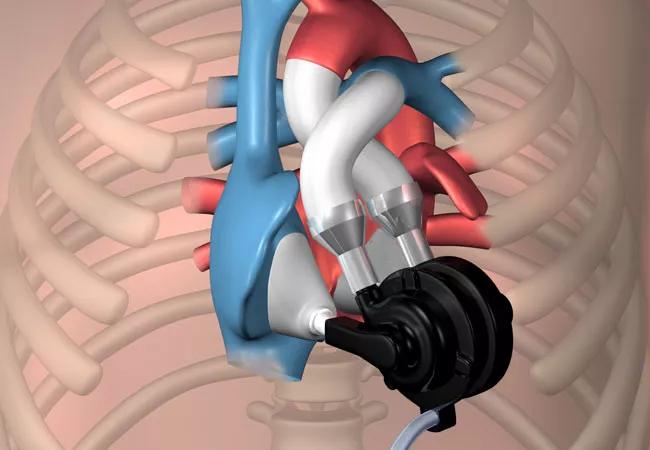
An LVAD is a mechanical pump that helps the heart circulate blood throughout the body. For patients who are not immediately eligible for transplant, it acts as a temporary support system—keeping them stable while they work on improving their overall health.
Rather than being a final solution, the LVAD creates a critical window of opportunity. It allows patients and care teams to address modifiable barriers and reassess transplant eligibility later.
What the Study Found
To better understand this process, researchers conducted a retrospective study involving 313 adult patients who received an LVAD between 2014 and 2021 at MedStar Washington Hospital Center.
By analyzing patient records, clinical data, and outcomes, the study aimed to track whether individuals could transition from being ineligible to eligible for transplant.
The results were promising:
- 60% of patients successfully resolved modifiable barriers after receiving an LVAD
- Many were able to move forward in their transplant journey
This highlights the real-world potential of combining medical technology with structured support systems.
A Journey That Isn’t Always Linear
The path to a heart transplant is rarely straightforward. Even after receiving an LVAD, challenges can still arise.
In fact, the study found that:
- 53% of patients developed new health concerns post-implantation
- Frailty was the most common issue, affecting 43% of patients
These findings emphasize the importance of continuous care, including proper nutrition, physical rehabilitation, and close medical monitoring.
Addressing Social and Racial Disparities
The research also shed light on disparities in healthcare access and outcomes.
- Black patients were more likely to face modifiable barriers (72% compared to 58% in non-Black patients)
- High BMI was the most common issue, often linked to broader social determinants such as access to healthy food and stable living conditions
Recognizing these differences is essential for creating more personalized and equitable care strategies.
The Power of a Team-Based Approach
One of the key takeaways from the study is that technology alone isn’t enough—success depends on collaboration.
A multidisciplinary care team plays a crucial role in helping patients overcome barriers. This team may include:
- Dietitians and bariatric specialists to support weight management
- Rehabilitation experts to improve strength and mobility
- Social workers and counselors to address housing and support systems
- Specialists like endocrinologists to manage chronic conditions such as diabetes
Together, these professionals create a structured pathway toward improved health and transplant readiness.
Looking Ahead: A Window of Opportunity
Modern LVAD devices, such as the HeartMate 3, can support heart function for several years, giving patients valuable time to improve their health and qualify for transplant.
This research reinforces an important idea: being ineligible for a transplant today does not mean being ineligible forever.
With the right combination of medical support, lifestyle changes, and coordinated care, many patients can turn a temporary setback into a second chance.
Final Thoughts
The journey to a heart transplant is complex and often unpredictable. But with tools like LVADs and a strong support system, patients have more opportunities than ever before to change their trajectory.
What begins as a “bridge to decision” can ultimately become a bridge to a longer, healthier life.