
“It’s Just Period Pain”… Until It Isn’t: Why Endometriosis Stays Unseen
She misses classes because the pain won’t let her move. Even getting out of bed during her period feels overwhelming. She stops asking for help, […]

She misses classes because the pain won’t let her move. Even getting out of bed during her period feels overwhelming. She stops asking for help, […]

Regular exercise plays a major role in overall health. It strengthens your heart, boosts energy, improves sleep, and even supports better mental well-being. But when […]
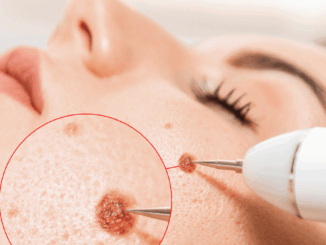
Most people have multiple moles—typically anywhere between 10 and 40—and they don’t all look or behave the same. One common type is the intradermal nevus, […]

For patients living with advanced heart failure, being told they are not eligible for a heart transplant can feel like the end of the road. […]

In recent years, a noticeable trend has emerged—girls are starting puberty and getting their first periods earlier than previous generations. What used to be considered […]

A bloated, heavy feeling in the abdomen around ovulation is something many women notice—but don’t always talk about. While it can be uncomfortable, it’s actually […]

George Nicolson are pleased to share with you an article included within the summer issue of The Scottish Decorators’ Federation magazine called Decorating Matters. Mental […]

More than 17 years ago, when Practo was founded, the goal was both simple and ambitious: to improve healthcare outcomes by making medical services more […]
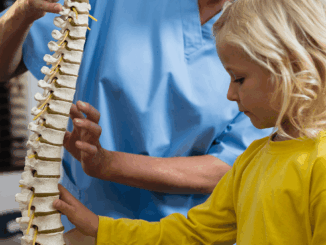
Diagnosing a posttraumatic tethered spinal cord typically relies on identifying a pattern of symptoms rather than a single definitive test. Physicians evaluate progressive changes following […]

Genetic testing has become one of the most powerful tools in modern cancer prevention. However, new research shows that important information from these tests does […]
Copyright © 2026 | WordPress Theme by MH Themes