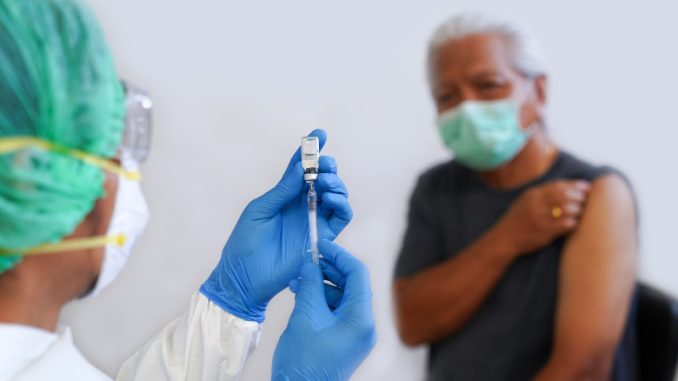
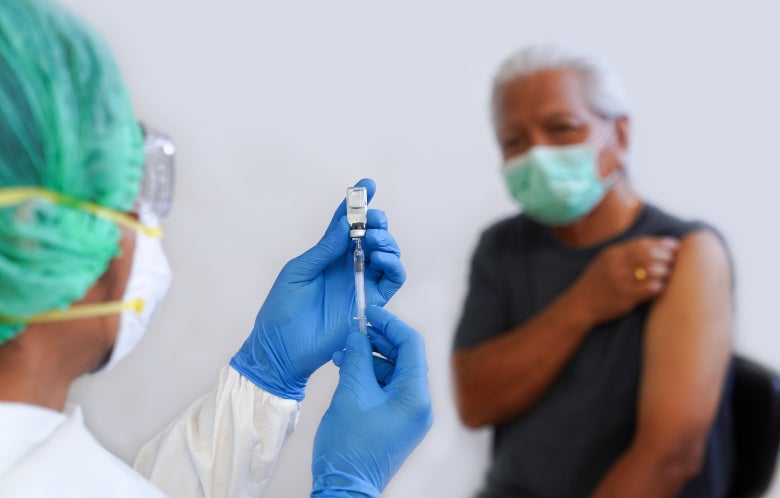
Israel began giving third doses of the Pfizer BNT162b2 mRNA vaccine against SARS-CoV-2 earlier this summer in response to the reported increased infectivity of the Delta variant. Amazingly, almost 50 percent of eligible senior citizens were given third dose booster vaccines within two weeks, allowing the health system to rapidly expand booster use to younger and less vulnerable populations. A study in the Lancet was recently published, describing this Israeli experience in real-time public health.
Researchers had access to data on 1,158,239 people eligible for a third vaccine dose as well as outcome data on hospitalization, a diagnosis of severe COVID-19, or death from the virus. Data analysis excluded people with prior COVID, health care workers, and those who were homebound or lived in residential living facilities but included people at high risk for severe disease. People receiving their third (booster) shot were matched seven days after the booster with another third-vaccine eligible person of similar age, sex, comorbidities, duration since completion of the original vaccine series, and number of prior COVID tests in the preceding nine months. Controls had all received two doses of the vaccine.
Results showed that three vaccine doses demonstrated effectiveness over two doses for all three primary outcomes: hospitalizations from COVID (93%; 231 events for 2 doses vs 29 events for 3 doses), severe COVID related illness (92%; 157 vs 17 events) and death from COVID (81%; 44 vs 7 events). This effectiveness spanned all ages studied, and observationally, it appeared that as the booster shots were given to younger and younger people, the population incidence of COVID-19 infections declined among those subgroups.
These numbers are very impressive, but we’d like to focus the discussion on one aspect of study design. Matched case control studies depend heavily on what is chosen as a matching criteria. In this case, time since the second vaccine dose and number of prior tests were chosen as a reasonable proxy to compensate for variations in health seeking behavior and concern about the disease. This adjustment assumes concern about disease is a primary factor in outcomes for vaccine preventable disease.
Is it? That the authors chose to specifically look at those who become severely ill or died from COVID is inarguably the most important set of outcomes, even though the outcome of actual infections is a close second. But vaccine uptake and effectiveness could be associated with a wide variety of other confounding determinants, from access to current health information and ability to navigate online sign-ups, to ability to take time off work for vaccination, to belief in unconventional treatments that may delay presentation of illness. These factors could each create differences within the two cohorts that affect outcomes separate from vaccination status. This study informs us about the potential impact of a third dose. However, as with all case control studies, no matter how well the cases are matched, the two groups are not prognostically equivalent at the outset and thus no causal relationship can be assured. There may be something inherently different about people who received the third dose that cannot be controlled for without randomization. That said, this well-executed observational study provides impressive evidence that a third dose provides additional protection against severe COVID-19 outcomes.
[“source=ebsco”]
